Newsletter
IND-Enabling Studies
Cell and Gene Therapy (CGT) drugs have their unique mechanism of action and require a more tailor-made approach for drug development and regulatory approval. Starting from custom cell line and animal model generation for the targeted disease, ASC’s multidisciplinary team of experts can develop preclinical assays to determine efficacy, pharmacodynamic, dose-ranging studies, biodistribution, and develop other IND-enabling assays to measure potency (AAV potency, DNA/ RNA/ protein levels) and toxicity of the drug in multiple species samples including NHPs, immunogenicity of the drug, and more. We will work with you every step of the way including pre-IND meetings with the FDA/ respective regulatory bodies to develop the right assay matrix for your CGT candidates.
Products and Services
Technical Details
Navigating the regulatory requirements for Cell and Gene Therapy (CGT) investigational drugs can be harrowing to say the least. With expert consultation and CRO resources provided by ASC, we can let you have a breather. ASC’s preclinical and IND-enabling assay development platform leverages our extensive expertise in cutting-edge molecular biology, cell biology, stem cell technologies to develop science-based, data-driven, pertinent assays for your early-stage CGT drugs. We will develop a customized assay matrix using a combination of several advanced techniques: quantitative PCR (qPCR), droplet-digital PCR (ddPCR), next generation sequencing (NGS), flow cytometry, ELISA, immunohistochemistry, western blotting, high content imaging, and more for a variety of preclinical requirements:
- Proof-of-concept studies: to determine feasibility and rationale for the clinical trial
- Pharmacodynamics: understand in vivo characteristics of the drug using customized assays to get predictive data for extrapolation to human subjects
- Efficacy and toxicity/ safety: to determine the effective of the drug in treating the pathophysiological condition it claims to treat; and characterize the product’s safety profile to determine risk-benefit ratio of the drug
- Dose ranging studies: to determine initial safe starting dose, dosing schedule
- Biodistribution: provides information on delivery, expression of gene therapy product/ engraftment of cellular therapies, distribution, persistence and therefore ensures a better understanding of the drugs’ activity and mechanism of action
- In vivo assay development: to enable translation of efficacy-safety data into clinical setting
- Immunogenicity assessments: develop assays to carefully measure and study the immunogenic potential of the cell or gene therapy candidate which would invalidate the treatment
- Custom assay development for any stage of your CGT pipeline including preliminary potency assays
Follow-up from your IND-enabling preclinical assays to our CMC consultation and support services for your non-clinical and clinical design, manufacturing and quality control for your biotherapeutics.
Application Notes
Clinical trials in gene and cell therapies have advanced rapidly in the past decade, reflecting significant advances in scientific innovation with better translation to clinical settings. Assessing the growth in this area of therapeutics, FDA anticipates that by the year 2025 they expect to approve 10-20 gene and cell-based therapy products a year.1 To date, majority of the gene therapies involving delivery to in vivo and ex vivo target cells (Ex. CAR-T), have utilized recombinant viral vectors such as adeno-associated virus (AAV), adenovirus, lentiviruses, vaccinia virus, and retroviruses. As with any therapeutic product developed for use in humans, an initial set of preclinical and non-clinical data aimed at assessing the risks/ safety and benefit/ intended efficacy profile is required. Preclinical (or non-clinical) studies that are conducted in a variety of in vitro (human cell lines) and in vivo (animal) models relevant to the targeted human system or disease, to gather as much safety and efficacy information can maximize the chance of success in human clinical trials.
In particular, gene therapies are highly specific to humans and therefore preclinical testing in human-relevant system is critical. And for virus delivery of gene therapy products, tissue infectivity (viral biodistribution of recombinant viruses) and viral shedding are assessments required by regulatory authorities.2 ASC’s genome editing experts can equip you with clinically relevant cell line or animal models as well as provide you with the technical expertise in designing preclinical assays for your gene therapy programs, such as assessing the right serotype of viral vector, biodistribution, viral shedding, virus titer (and dose determination), potency assays and more.
Example of Pharmacodynamic (PD) Study to Evaluate CRISPR/Cas9 Genome Editing Efficiency of a Recombinant Adeno-Associated Viral Vector
In Vitro Indel detection using droplet digital PCR (ddPCR) following CRISPR-SaCas9 genome editing at a specific genetic locus of choice in HEK293T cells
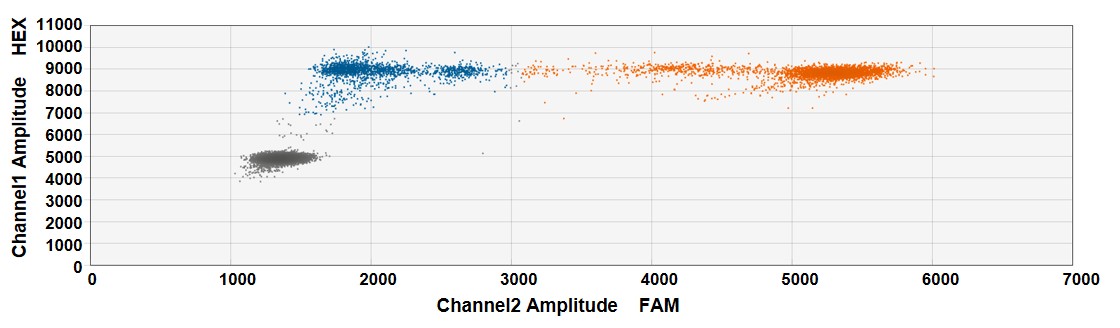
Figure. HEK293T cells in 12-well cell-culture plates were co-transfected with 0.5µg CMV-SaCas9 plasmid and 1µg U6-GuideRNA plasmid (1:2 ratio) using Lipofectamine3000. Indel detection at the locus was done by ddPCR using NHEJ genome editing detection drop-off assay (Bio-Rad) 48 hours post-transfection. The assay included one set of primers and two probes annealing the amplicon (FAM-labeled Reference probe and HEX-labeled Drop-off probe). Indel (blue, 37.6%) and unedited (orange) amplicon droplet populations are indicated. Gray droplets population includes droplet with no target sequence.
In Vivo knock-in detection in tissue samples at a specific genetic locus in a Humanized mouse model using ddPCR following CRISPR-SaCas9 genome editing
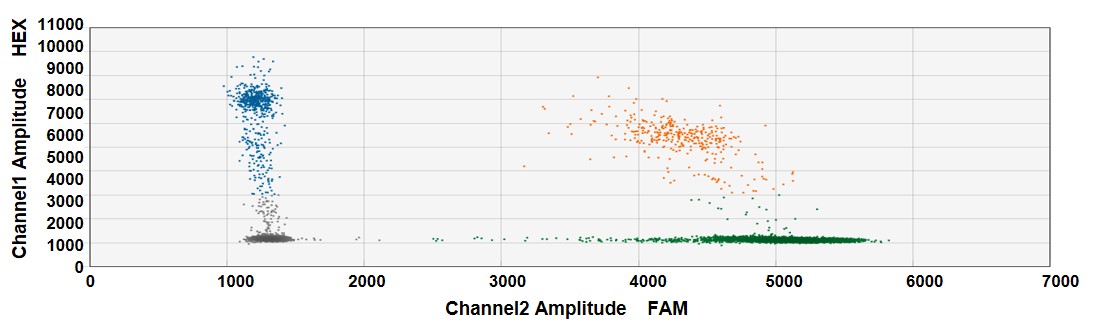
Figure. Knock-in abundance following CRISPR-SaCas9 genome editing at a specific genetic locus of choice in C57BL/6 WT mouse. Combined delivery of two recombinant AAV viruses containing the gene of interest and SaCas9-GuideRNA was applied at a total dose of 1.8E+11VG/Kg. To determine the knock-in abundance, two ddPCR primer-probe assays were used: the first assay includes a primer set that amplifies the target locus only following insertion (targeting the junction of insertion), and a FAM-labeled probe. The second assay, including a HEX-labeled probe, targets a reference region and is used to count all genome copies. KI abundance is calculated by the ratio of FAM-positive droplets (KI amplicons) to all HEX positive droplets (Reference amplicons). Gray droplets population includes droplet with no target sequence. KI% detected here is 10%.
Examples of Assay Development for a Recombinant Adeno-Associated Virus
Viral biodistribution in mouse tissue (solid tissue)
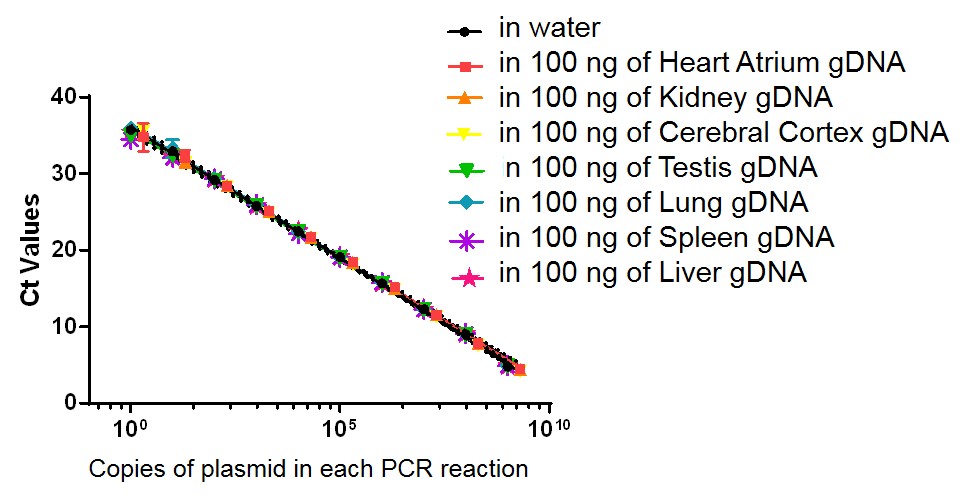
Figure. Standard curve developed to measure viral biodistribution for a recombinant adeno-associated viral (AAV) vector in mouse tissues. Genomic DNA (gDNA) sample from various tissues (heart, kidney, cerebral cortex, testis, lung, spleen, and liver) was extracted from PBS-only injected C57BL/6wild type (WT) mouse tissues, and added to a serial dilution of plasmid containing the gene of interest. Quantitative PCR (qPCR) was performed to generate a standard curve for the biodistribution of the gene of interest. Assay sensitivity: ≤50 copies of plasmid per 1 μg gDNA from mouse tissue. Note: No signal was detected in all negative controls (non-plasmid samples with and without tissue gDNA).
Virus shedding in human fluid samples
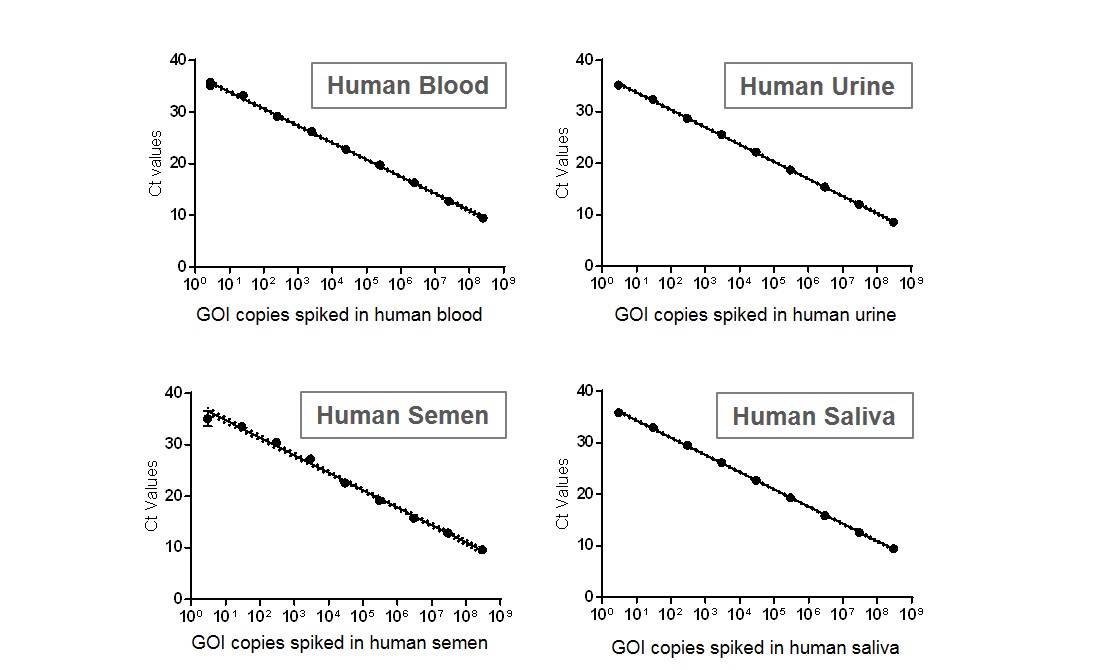
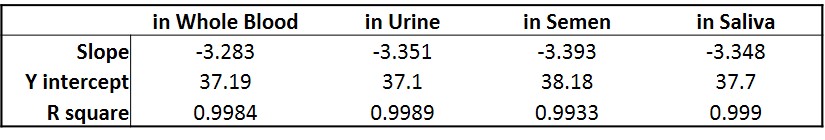
Figure. Standard curve developed to measure viral shedding of a recombinant adeno-associated viral (AAV) vector in human body fluid samples. A serial dilution of plasmid containing the gene of interest was spiked in various human body fluid samples (blood, urine, semen and saliva), and the DNA (both viral DNA and gDNA, if possible) was then extracted. Quantitative PCR (qPCR) was performed to generate a standard curve to measure viral shedding. Note: No signal was detected in all negative controls (DNA extracted from normal human body fluid samples without plasmid spiked-in).
1. U.S. Food & Drug Administration. (2019). Statement from FDA Commissioner Scott Gottlieb, M.D. and Peter Marks, M.D., Ph.D., Director of the Center for Biologics Evaluation and Research on new policies to advance development of safe and effective cell and gene therapies. Retrieved from https://www.fda.gov/news-events/press-announcements/statement-fda-commissioner-scott-gottlieb-md-and-peter-marks-md-phd-director-center-biologics
2. MacLachlan, T. K., McIntyre, M., Mitrophanous, K., Miskin, J., Jolly, D. J., & Cavagnaro, J. A. (2013). Not reinventing the wheel: applying the 3Rs concepts to viral vector gene therapy biodistribution studies. Human Gene Therapy Clinical Development, 24(1), 1-4.
Support Materials
Publications
Cell and Gene Therapy Applications:
- Chen, H., Shi, M., Gilam, A., Zheng, Q., Zhang, Y., Afrikanova, I., ... & Chen-Tsai, R. Y. (2019). Hemophilia A ameliorated in mice by CRISPR-based in vivo genome editing of human Factor VIII. Scientific reports, 9(1), 1-15.
Other CRO Services:
- Mace, E. M., Paust, S., Conte, M. I., Baxley, R. M., Schmit, M., Mukherjee, M., ... & Akdemir, Z. C. (2019). Human NK cell deficiency as a result of biallelic mutations in MCM10. bioRxiv, 825554.
- Baskfield, A., Li, R., Beers, J., Zou, J., Liu, C., & Zheng, W. (2019). Generation of an induced pluripotent stem cell line (TRNDi004-I) from a Niemann-Pick disease type B patient carrying a heterozygous mutation of p. L43_A44delLA in the SMPD1 gene. Stem cell research, 37, 101436.
- Hong, J., Xu, M., Li, R., Cheng, Y. S., Kouznetsova, J., Beers, J., ... & Zheng, W. (2019). Generation of an induced pluripotent stem cell line (TRNDi008-A) from a Hunter syndrome patient carrying a hemizygous 208insC mutation in the IDS gene. Stem cell research, 37, 101451.
- Cheng, Y. S., Li, R., Baskfield, A., Beers, J., Zou, J., Liu, C., & Zheng, W. (2019). A human induced pluripotent stem cell line (TRNDi007-B) from an infantile onset Pompe patient carrying p. R854X mutation in the GAA gene. Stem cell research, 37, 101435.
- Yang, S., Cheng, Y. S., Li, R., Pradhan, M., Hong, J., Beers, J., ... & Zheng, W. (2019). An induced pluripotent stem cell line (TRNDi010-C) from a patient carrying a homozygous p. R401X mutation in the NGLY1 gene. Stem cell research, 39, 101496.
- Baskfield, A., Li, R., Beers, J., Zou, J., Liu, C., & Zheng, W. (2019). An induced pluripotent stem cell line (TRNDi009-C) from a Niemann-Pick disease type A patient carrying a heterozygous p. L302P (c. 905 T> C) mutation in the SMPD1 gene. Stem cell research, 38, 101461.
- Huang, W., Xu, M., Li, R., Baskfield, A., Kouznetsova, J., Beers, J., ... & Zheng, W. (2019). An induced pluripotent stem cell line (TRNDi006-A) from a MPS IIIB patient carrying homozygous mutation of p. Glu153Lys in the NAGLU gene. Stem Cell Research, 101427.
- Sundararaj, K. P., Rodgers, J., Angel, P., Wolf, B., & Nowling, T. K. (2020). Neuraminidase activity mediates IL-6 production through TLR4 and p38/ERK MAPK signaling in MRL/lpr mesangial cells. bioRxiv.
- Li, R., Baskfield, A., Lin, Y., Beers, J., Zou, J., Liu, C., ... & Zheng, W. (2019). Generation of an induced pluripotent stem cell line (TRNDi003-A) from a Noonan syndrome with multiple lentigines (NSML) patient carrying a p. Q510P mutation in the PTPN11 gene. Stem cell research, 34, 101374.
- Li, R., Pradhan, M., Xu, M., Baskfield, A., Farkhondeh, A., Cheng, Y. S., ... & Rodems, S. (2018). Generation of an induced pluripotent stem cell line (TRNDi002-B) from a patient carrying compound heterozygous p. Q208X and p. G310G mutations in the NGLY1 gene. Stem Cell Research, 101362.
- Poli, M. C., Ebstein, F., Nicholas, S. K., de Guzman, M. M., Forbes, L. R., Chinn, I. K., ... & Coban-Akdemir, Z. H. (2018). Heterozygous Truncating Variants in POMP Escape Nonsense-Mediated Decay and Cause a Unique Immune Dysregulatory Syndrome. The American Journal of Human Genetics, 102, 1-17. https://doi.org/10.1016/j.ajhg.2018.04.010
Vozdek, R., Long, Y., & Ma, D. K. (2018). The receptor tyrosine kinase HIR-1 coordinates HIF-independent responses to hypoxia and extracellular matrix injury. Sci. Signal., 11(550), eaat0138.
FAQs
What is droplet digital PCR (ddPCR)?
Does you have experience with experiments that use AAV? If yes, what type of studies?
Would you be able to use FACS (Flow cytometry) for assays using AAV vectors that express GFP?


_L1.jpg)
